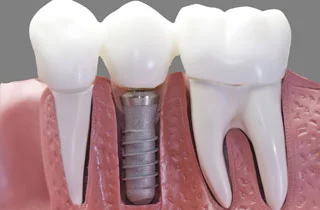
Dental implantation is a surgical procedure. Every procedure carries a certain risk of complications; similar problems can arise in connection with the placement of dental implants. To put your mind at ease, let us preface by saying: more than 95 percent of dental implant procedures proceed without any problems. With proper care of the implant (or implants), this success rate can be increased to over 98 percent. Therefore, in our article, we shed light on the less than two percent of cases where this dental procedure, which is constantly being developed through new materials and technologies, is not entirely successful. The aim of this article is to objectively, yet in a reassuring tone, explain the potential problems associated with dental implants and how to avoid them.
Although the problems that can occur with a dental implantation affect only a few people (see introduction), they are still of great importance. A conscientious specialist must deal with the problems of each individual patient competently. From this article, you can learn about the rarely occurring, but possible complications. You may encounter the terms, meanings, and in some cases, the prevention and resolution methods.
Our article deals with the potential complications of dental implants:
- Why did my body reject the dental implant?
- What is the biggest reason implants fail?
- Who shouldn’t get a dental implant? Contra-indications
- How long does it take for a dental implant to reject?
Why did my body reject the dental implant?
Failure of osseointegration
Osseointegration refers to an appropriate functional and structural connection between the implant and the supporting bone tissue. This process takes on average a few months. A common cause of an unsuccessful implantation is that the jawbone and the implant root cannot properly connect. The implantation is considered a failure if the implant moves, fails, or exhibits bone loss of more than 1 mm in the first year, or dental bone loss of more than 0.2 mm in the second year after implantation. The failure of osseointegration can be due to, among other things, incorrect positioning of the implant, insufficient bone density or bone quantity, overloading, injury to the tissue around the implant, possible external force, or rarely, a broken or fatigued implant. Read more about prevention of bone loss
In the case of patients where the supporting bone surface is not sufficiently high, wide, or long, a sinus lift, or the associated bone augmentation, can help. However, these supplementary procedures increase both the duration of the dental implantation and the costs.
It must also be mentioned here that tooth deficiency reduces bone substance, as the chewing force load is absent in these areas. Patients who have lived months or years without teeth often need a bone augmentation before the placement of the implants.
Damaged nerves and/or tissues (very rare dental implant problem)
Another, but very rare complication, is damage to the nerves and tissues around the implant, particularly injury to nerves. If the implant is placed too close to the nerve, the patient can experience chronic pain, or the face, gums, tongue, lips, and jaw can sting and tingle. The nerve damage can be temporary or permanent. As a last resort, removal of the implant may prove necessary to resolve the problem. Based on experience, this complication is caused in almost all cases by a treatment error of an implantologist without sufficient practical experience.
Minor damage to the tissue, however, is normal. Slight bleeding and pain can still occur for a few days after the surgery. In case of extremely severe pain, or heavy bleeding that does not subside even a few days after the surgery, one must visit the dentist, implantologist, or stomatologist.
Dental implant complications: overloading
Complications can also occur if the implantologist decides, although it is not recommended, to perform the entire dental implantation procedure in one stage. This means that they immediately screw the abutment into the implant placed in the jawbone and also attach the crown. The usual, two-stage procedure allows the implant enough time to properly connect with the bone before the components above the gums – i.e., the abutment and the crown – are attached. The advantage of the one-stage procedure – if none of the aforementioned problems occur – is that the surgical aftercare can be shorter, the recovery faster, and the follow-up treatment shorter.
Overloading the implant is also a risk for complications. This can occur when too much pressure is exerted on the components above the gums – the abutment and the crown. This influence, these forces, can interrupt the process of osseointegration, i.e., the structural and functional connection of the implant with the supporting bone. The one-stage implantation procedure is not recommended for patients who have insufficient (low) bone substance.
When replacing teeth in the upper jaw, the problems of the sinus floor present the greatest challenge to the implantologist. The condition of the sinus floor and problems with the quantity and quality of the posterior jawbone can make tooth replacement with implants in these areas difficult.
To achieve a thickening of the sinus floor, the implantologist may opt for a sinus lift. This means that the existing bone substance is lifted to prepare adequate space for bone augmentation. The procedure achieves the building of sufficient bone substance that accommodates and long-term supports the foundation for the artificial teeth. The patient must be informed in a timely manner, before the start of the implantation, about the potential problems with the sinus floor. Further advice on problems after bone augmentation and on problems after sinus lift
Dental-implant rejection
Like other implants (artificial materials implanted in the body), dental implants can also be rejected and expelled by the body. In this case, the human body does not accept the material of the substructure of the dental implant; it simply does not fuse with the bone. Rejection is not actually a cause, but rather one of the possible consequences of the problems listed in our article: inadequate quality of the implants, a poor specialist, or another illness of the patient can cause this.
Complications due to faulty implants(e.g. breaking or crooking)
Although the substructure (the implant) is made of metal, usually titanium, it can fatigue or break. Nowadays, this problem is less relevant thanks to redesign and the use of even better base materials, but it can still occur. The implant can also break due to external force. For example, through a violent blow to the face or through overloading over a longer period, such as teeth grinding, clenching teeth, or overloading due to an unbalanced chewing surface.
Allergic reactions
The implants are made from titanium alloys, but they contain traces of nickel. Although very rare, some patients can have an allergic reaction to titanium. In others, inflammatory reactions can occur. The symptoms are highly variable, from itching to chronic fatigue. The MELISA test is the only scientifically founded method for determining whether and to what extent someone is truly allergic to titanium.
Bad professional
Although the choice of a poor specialist is at the end of the list, it is the most common reason for the rejection of implants. A good specialist is known for their knowledge, carefulness, and appropriate hygienic environment. Their business card is always passed around. Read more about Dental Implant Manufacturers
What is the biggest reason implants fail?
With implants, inflammatory symptoms are one of the most frequently occurring complications of dental implantations. Peri-implantitis refers to the inflammation of the soft and hard tissues around the implant. This can occur if bacteria are present in the area to be operated on during the placement of the implants. Later, it can also occur if the implants and their surroundings are not properly cared for. This type of inflammation can also be caused by the crown cement if it emerges from under the crown during fixation and gets into the gum.
Peri-implantitis is the most common reason for inflammation of the bones around the gum and/or around the dental implant. This inflammation is more likely to occur in patients with diabetes, thin gums, or insufficient oral hygiene. The prospects of a successful dental implantation are significantly diminished in this sense, particularly by smoking.
Peri-implantitis is rare in itself, but it is important to recognize the symptoms early and treat them immediately. With a good specialist and by maintaining appropriate oral hygiene, this risk can be minimized.
Who shouldn’t get a dental implant? Contra-indications
Furthermore, there are numerous circumstances and external factors that justify the rejection of tooth replacement by implantation on the part of the implantologist. The following exclusion criteria must certainly be considered:
- the route of the main nerve in the lower jaw cannot be safely located
- insufficient bone mass, the bone structure is not wide enough or large enough
- type 2 diabetes when non-treated,other illnesses (serious cases of heart, oncological or other diseases)
- teeth grinding (bruxism)
- bad hygienic circumstances, lack of cooperation from the patient
- returning gingivitis
How long does it take for a dental implant to reject?
Early Rejection:
Occurs within the first 3-4 months after implant placement. Causes: Surgical error, Infection, Poor oral hygiene, Smoking, Uncontrolled diabetes or autoimmune diseases.
Late Rejection:
Can occur months or even years after the initial implant placement. Causes: Peri-implantitis, Excessive biting forces, Poor oral hygiene, Trauma.
Signs of Implant Rejection
Persistent and increasing pain around the implant site. – Gums around the implant are red, swollen, and tender. – The implant feels mobile or wobbly. – Gums recede, exposing the implant. – Presence of pus or a bad taste around the implant. – Discomfort or pain when biting down.
Important Notes: If you suspect implant rejection, contact your dentist immediately. Early intervention can often save the implant.
Through early intervention, the implant can often be saved. We have reached the end of our long, frightening list. This listing gives the impression that the placement of artificial teeth is prevented and complicated by numerous factors. At the end of our article, however, we would like to emphasize again that only a small number of cases are affected by these complications. In more than 95 percent of implantations, the procedure is successful. Seek out a good specialist with whom a successful implantation is guaranteed! More information on Repairs of Dental Implants